Moving forward with Rural Surgical Networks
Port McNeill doctor installed as CMA's 149th president - Granger Avery
Report on AGM featuring Deputy Minister Stephen Brown's address
NewsFlash
Suicide prevention toolkits now available
Salt Spring Island Local Action Team has developed three suicide prevention toolkits targeting youth, adults and professionals. The toolkits include local contact information, telephone and web resources, as well as practical tools for identifying who’s at risk and creating treatment strategies and action plans. You may adapt the toolkits to your community by contacting Janine Gowans at the Salt Spring Island Chapter.
Gabriola goes all out during mental illness awareness week
Gabriola’s local Health and Wellness Collaborative, an A GP for Me initiative, sponsored three days of events during mental illness awareness week in early October. The events included a half-day workshop on how to help people at risk of suicide; various meet-and-greets; drop-in consultations with mental health nurses, physicians and social workers; and facilitated discussions on a range of mental health issues.
Increasing access to mental health services to island communities
Engagement and planning, funded by Shared Care, is to begin in November 2016 among Northern Gulf Island, Gold River, Island Health, Gabriola and two other Divisions of Family Practice in the development of an integrated system of care for Rural Residents with MHSU needs. This initiative is intended to support and enhance services and leverage psychiatric and counselling services through the use of telehealth.
Jel Coward is one of 5 new physician representatives to the GPSC
The representatives were recruited through heath authority-based interdivisional CSC tables across the province. The role is to represent physician voices rather than the specific Divisions' views, and is set for a 4 month period with evaluation of the new system by the GPSC. Jel is excited for the opportunity to bring further rural and remote physician perspectives to the GPSC.
THE LONG READ.....
Back to the future: Moving forward with Rural Surgical Networks
Bob Woollard remembers fondly a Christmas in Clearwater several years ago.
But not for typical yuletide reasons. Rather, at the centre of this particular memory is Clearwater’s little 10-bed hospital. “Five babies were born that Christmas,” says Woollard. “The ward was full with babies and their moms.”
“Those were better times,” observes Woollard, now associate director of the Rural Coordination Centre of BC and professor in UBC’s Department of Family Practice, reflecting on his 16 years as a rural doctor in Clearwater. “We used to deliver 100 babies a year there, and now no planned deliveries are done at all.”
Sadly, Clearwater isn’t the only community in BC to lose that capacity. “There’s been a dramatic attrition of obstetrical surgical services—and a loss of decision-making in rural and remote communities across Canada—due to the forces of centralization and specialization,” says Woollard.
“An increasing number of women—and aboriginal women are over-represented here—have to travel to deliver their babies.” - Bob Woollard, Associate Director, Rural Coordination Centre of BC
“Over time, obstetrical services were bled away to larger regional hospitals,” he says, “leaving small communities unsupported. And today, urban specialists control the training and delivery of secondary care—including maternity care and operative delivery.”
The numbers speak volumes: In 1995, there were 20 small surgical service facilities in BC like the one that used to serve Clearwater. Today, that number has dwindled to 11.
“Resource-based towns where workplace injuries are an issue need sound trauma services. Without them, you end up bleeding away the lifeblood of the community.” - Bob Woollard, Associate Director, Rural Coordination Centre of BC

|
Dr. Bob Woollard with one of his littlest family members
It’s not just about maternity care either. “Surgical and obstetrical services are entwined at the hip,” says Woollard. “It’s not a matter of doing the occasional C-section. You need an entire OR team on hand. You can’t provide urgent responses without other surgical services. Resource-based towns for example, where workplace injuries are an issue, need sound trauma services. Without them, you end up bleeding away the lifeblood of the community.”
Fortunately, Woollard and others who are equally passionate on the subject are working hard to implement a solution, starting with an October 2015 joint position paper on rural surgery and operative delivery.
In a nutshell, says Woollard, “The joint paper describes the fact that to provide a robust rural surgical infrastructure, you need a networked system of specialist-generalist surgical care services, with a virtual case room.”
The network model
The network model calls for BC’s rural and remote communities to develop strong human relationships and networks of care with each other and with nearby regional centres. These relationships are crucial, says Woollard, because they transcend geography and the boundaries between clinic, hospital and ER.
Care providers would work together, connecting electronically for shared consultations or training sessions. “And the folks on the frontlines would feel supported like I did in Clearwater,” says Woollard. “I never felt like someone was going to pull the rug out from under me when something went wrong.”
And that feeling of support, Woollard says, whether through virtual connection or in real-time, is crucial for recruitment and retention.
In January, 2016, a summit on Rural Surgery and Operative Delivery took place in Banff to further the network model. Woollard says its goals were threefold:
- To broaden the coalition that issued the Joint Position Paper;
- To reset the work plan going forward around consensus on networks of care, credentialing/privileging, C-section training and organization for action, and;
- To consider the location, membership, mandate and resources of a national initiative that will expand the stakeholder base.
Reason for optimism
Today, Woollard is cautiously optimistic: “We have provincial input, we have input from the five health authorities, we’ve identified the necessary elements for change, and we have this wonderful organization called the Rural and Remote Division. We’ve created the conditions to make things happen; now it’s up to the members of the Division. To truly thrive, the networks central to solving the problem have to be based in rural communities.”
Fortunately, there are reasons on the frontlines to be hopeful.
Rural health providers already have a tradition of working in teams to provide quality, safe, customized care to patients, says Woollard. And now, supported by the Rural and Remote Division, they can grow, nurture and legitimize the networks of care described in the position paper—ultimately, increasing the capacity of the health care system as a whole.
A solid starting point in Revelstoke/Lillooet
Some rural communities, like Revelstoke and Lillooet—the latter being the smallest remaining rural surgical site in the province—are already well on track to achieving an effective network model. In both communities, surgical, maternity and trauma care services are being networked to form a comprehensive, integrated regional team.
“Both communities have some elements of a surgical services network in place now and we’re a great place to start to optimize the network model,” says Vikki Vogt Haines, one of three GP surgeons practicing in Revelstoke. “I’d say Revelstoke is about halfway there.”
Currently Haines and her colleagues deliver 80 to 100 babies each year, about 25 percent of those by C-section. Lillooet has a full-service maternity program with intermittent C-section coverage, which allows 55 to 60 percent of moms to deliver locally.
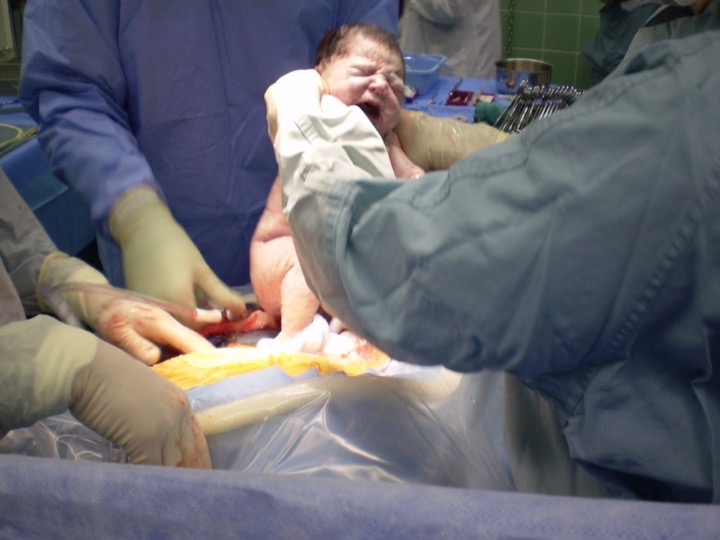
|
Physician lead Nancy Humber delivering a baby by
C-Section in Lillooet's fully-equipped operating theatre.
Likewise, patients from other communities in the network, both large and small, from Vernon to New Denver, can be referred to Revelstoke for simple elective procedures, reducing wait times in the Health Region. Revelstoke surgical wait times are typically one to two months, compared to three to four times that in larger centres.
With six acute care beds, Lillooet is networked with Kamloops, its closest referral centre, as well as nearby Lytton and Ashcroft. “We already work in integrated highly effective teams,” says long-time Lillooet rural doctor Nancy Humber, “and now we’re looking to pair with regional integrated teams of care.”
"The patient never has to travel. The consult and procedure are done on the same day in their own community." - Nancy Humber, Lillooet
Humber says for complicated surgical patients, she can phone the general surgeon in Kamloops, triage the patient, book the surgery in Lillooet, to be done either by her, the general surgeon, or the two of them as a team. “The patient never has to travel. The consult and procedure are done on the same day in their own community.”
And doing these elective surgeries allows Haines and Humber and their colleagues to hone their surgical skills.
“In places that are too small to support resident specialist services, surgical programs like the ones in Revelstoke and Lillooet are a foundational piece in a sustainable rural health site,” says Humber, “particularly as they serve populations that are vulnerable and often culturally and geographically isolated. And increased access to care in sustainable models is important for the region’s general population health.”
Still, the surgical facilities in both Revelstoke and Lillooet are under-utilized. “For three days each week,” says Haines, “we have a great OR facility that’s not being used.” And that can impact patient care and physician recruitment and retention, she says, “because practitioners feel the burden of on-call services, yet the balance of enough elective cases to maintain proficiency can be tenuous. Fluctuations in service delivery aren’t good for patients or doctors.”

“…we’re a great place to start to optimize the network model. I’d say Revelstoke is about halfway there.” - Vikki Vogt Haines, Revelstoke
Complicating matters in Revelstoke is the fact that the population swells by up to 6000 in ski season, and recently, by almost as many in the summer months. “This is an attractive recreational community and it tends to bring in people who are doing potentially risky activities like skiing, hiking and biking,” says Haines.
It’s a phenomenon reflected in the stats. From 2011 to 2015, ER visits in Revelstoke rose 17 percent. “We either improve our surgical services networks,” says Haines, “or we’re unprepared for the numbers.”
Vikki Vogt Haines, Revelstoke
In the short-term, next steps for both communities are to enhance clinical coaching and training opportunities for anesthetists, ESS and OR Nurses, a process that has already begun in partnership with RCCbc and the University of BC; and to enhance remote presence technology that will allow rural doctors separated by distance to collaborate with specialists in clinical settings.
In the longer term, say Haines and Humber, continuing the work will require additional funding and partners.
But it’s well worth it for all the stakeholders, says Humber: “For the province, it’s an opportunity to be a leader both nationally and internationally on an important shared issue. For rural doctors, it means enhanced quality of life and the ability to better care for our patients. And for patients, it means having their health care needs met in their communities—by providers they know and trust.”
Former Port McNeill doctor installed as CMA's 149th president
He’s known as the pride of Port McNeill, with a list of achievements almost as long as a Tolstoy novel: four decades as a rural doctor in Port McNeill, a 35-year teaching career at UBC, and stints as president of the BC Medical Association (now Doctors of BC), executive director of the RCCbc, and co-chair of the Joint Standing Committee on Rural Issues, to name just a few.
The 70-year-old Granger Avery can now add to that list President of the 80,000-member strong CMA. He was installed as President on August 24—only the 13th BC doctor to hold the position—during the CMA General Council, at which he gave an inspiring inaugural address.
Avery began his speech by pointing out that Canada’s health care system is not keeping pace with the present and future needs of Canadians, slipping to 10th of 11 similar developed countries in terms of timeliness, efficiency and safety.
He made reference to the bleak health outcomes of Canada’s aboriginal people and he called for the following measures:
. An increased role for patients and family caregivers in the care process;
. Widespread support for the social determinants of health and healthy living, and;
. Enhanced collaboration among government, health professionals, academics, health care managers and
the public, especially aboriginal people.
The CMA is the organization to broker such a “true health collaborative,” Avery said.
He ended by urging everyone to get involved and stay united as a profession.
 Here is just a sampling of the many quotable moments of Avery’s address:
Here is just a sampling of the many quotable moments of Avery’s address:
“I have come to observe again and again that things learned—and taught—in rural practice often have broad application in urban and larger environments.”
“Our profession is blessed with a plethora of talented, hard-working, dedicated and thoughtful practitioners. Together we can accomplish the change that returns Canada’s health care system to its rightful place as a world-leader.”
“…we must not be afraid to step up and lead the way toward a better future, working with our other health care partners. Let us think big.”
Dr. Granger Avery
Back to headlines >
Report on AGM featuring Deputy Minister Stephen Brown's address
About 60 people from 15 BC communities linked in virtually to participate in the Rural & Remote Division’s 2016 Annual General Meeting on September 27, featuring Deputy Health Minister Stephen Brown.
The evening began with a warm welcome from our Board Chair Rebecca Lindley, who described Rural and Remote Division as “physicians from a collection of smaller communities across BC that share challenges and work together to make a difference in patients’ lives.”

The Deputy Minister acknowledged that a “virtual” meeting was an appropriate way to discuss the realities of rural health care.
Here is some of what he had to say:
“Rural and remote communities need to be the most innovative because the reality is that some services will never be located in smaller communities.”
Deputy Minister Stephen Brown addresses attendees,
remotely and in-person, at the 2016 AGM.
“We need full-service family practices, where care providers collaborate and work together. This isn’t a challenge to you rural doctors because that’s what you do anyway.”
“I recently met with several residents, who said they wanted to practice full service medicine and they wanted mentoring. You do both brilliantly.”
“Maintaining a continuing dialogue [with rural physicians] is important to creating a change network.”
“We need to look at new strategies for communicating and connecting, including face-to-face and virtual communications channels. We need a more coherent virtual strategy and we need the organizational capacity to support broad generalist practice. We also need to simplify funding to make it more flexible for doctors so that you can concentrate on clinical care.”
“Health authorities that encompass rural and remote communities need to start showing leadership around the rural health agenda. We need to take rural health to the next level. We need to network with rural physicians to better figure out ways to link the health authorities into the process.”
After Stephen Brown’s comments, Board Chair Rebecca Lindley, gave an overview of Rural and Remote Division’s strategic position of supporting change at the local level, while fostering partnerships and a rural voice at regional and provincial levels.
Three of our physician leaders provided insights into key initiatives within and across our communities. Carrie Marshall from Long Beach, and David Whittaker from Port McNeill, talked about how their communities are leading change relating to rural and remote primary care. Both highlighted challenges of geography, and transportation. They emphasized how primary care home is evolving in their communities through patient-centred and longitudinal care, while leveraging inter-professional teamwork and technology.
Lillooet’s Nancy Humber gave a lively slide presentation—featuring stunning photography by colleague Ian Routley—on rural surgical networks. She explained why networks are vital to rural health services and described the opportunities through coaching, connections across communities and the use of technology in supporting rural surgical services.
The evening ended with a short question and answer period moderated by our Treasurer David Butcher, followed by the business meeting.


