Salt Spring Teledermatology Initative
2016 Rural Emergency Continuum of Care Conference
Gabriola's Most Vulnerable Benefit from Social Worker Position
Adult Day Program Fills Gap in Care
2nd Annual Rural Locum Forum Reflects Supportive Locum Community
Telehealth
Salt Spring Teledermatology Initative:
The Benefits of Early Diagnosis Without Leaving the Support of Community
It’s no bigger than a cell phone, but its potential impact on family doctors and patients in BC’s rural and remote communities is sizeable.
It’s called a dermascope and it’s part of a Shared Care teledermatology initiative on Salt Spring Island led by Salt Spring Island doctors Shane Barclay and Paula Ryan.
The initiative, based on use of the dermascope and BCConsultDerm, a secure website platform for sending images remotely, addresses the challenges of delivering health care services like dermatology to BC’s smaller communities.
Peace of Mind for Patients
Using the combined technology, doctors can identify quickly skin lesions that may be malignant and require biopsies or treatment. Patients get the peace of mind that comes with a diagnosis—without long wait times or the disruption of travel to and from larger communities with more resources.
Science is Simple
The science involved isn’t complicated says Dr. Ryan, who learned about dermascopy at a conference in Arizona two years ago. “I thought then, ‘Wow, we should be using this at home.’”
Fast forward a couple of years and, after a one-day training workshop arranged by Dr. Ryan, 10 of the 11 doctors on Salt Spring are using the dermascope as a standard part of their practice.
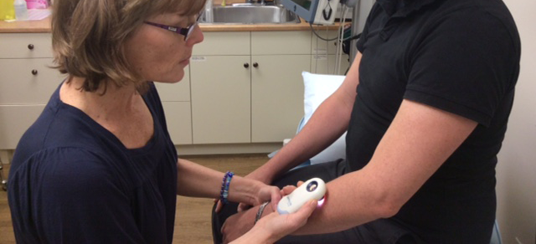
Here’s how the technology works. The dermascope uses magnified polarized light to reveal structural details in skin lesions or rashes. “It allows us to make better judgments about follow-up treatment, whether a biopsy is required or whether we need to get a dermatologist involved,” says Dr. Ryan.
If it’s determined that a dermatologist is required, Dr. Ryan and her colleagues simply take a picture of the lesion using a special adaptor on the dermascope. They then send the magnified image to one of 11 dermatologists across the province via BCConsultDerm.com.
The magnified image allows the dermatologist to more accurately identify possible malignancies, especially when looking at pigmented lesions, which are difficult to diagnose using only the telederm platform. The web platform has facilitated more than 2000 consults since 2011, with a turnaround time of about 48 hours.
While new in BC, dermascopy used within the framework of teledermatology, has been proven effective for early diagnosis of melanoma in Australia and New Zealand. Both countries now boast some of the best patient outcomes for melanoma in the world.
As doctors in other small communities like Salt Spring receive training on the dermascope and in teledermatology, Dr. Ryan hopes BC will follow suit.
2016 Rural Emergency Continuum of Care Conference:
From Airway Management and Suturing to Obstetrics and Telehealth
As a former doctor in BC’s small northern community of Fraser Lake, Dr. John Pawlovich learned early on the benefits of using technology to deliver health services.
Dr. Pawlovich is just one of the presenters at this year’s Rural Emergency Continuum of Care conference coming up on June 9 and 10 in Prince George. He and fellow telehealth advocate Dr. Michael Jong, from the Northern Family Education Program in Newfoundland and Labrador, “will provide lots of examples of how telehealth can support rural and remote emergency care,” says Dr. Pawlovich.
Involving live video conferencing and store-and-forward capability for transmitting images, the telehealth technology is relatively simple, yet has multiple applications, Dr. Pawlovich says. A specialist in another community can view a live ultrasound from Prince George or an echo cardiogram of a baby’s heart in Port Alberni, for example. Or doctors in one community can talk to patients and their health teams in another in real time and vice versa.
“Using telehealth is like being at the bedside,” Dr. Pawlovich says.
Today, as program coordinator for Rural Education Action Plan (REAP) BC, Dr. Pawlovich travels the province showing health care providers in rural communities how technology can support people on the ground. “We support education for rural physicians and students and residents who want an experience in rural communities. Telehealth is a big part of that education.”
Following Dr. Pawlovich’s presentation at the conference, RCCbc, REAP and the Rural and Remote Division’s Telehealth Steering Committee will co-host a telehealth engagement meeting. The meeting is an opportunity for physicians in rural and remote communities to discuss how to strengthen the rural physician’s voice in telehealth service development across BC.
Dr. Pawlovich and Dr. Jong will also run a telehealth workshop for those who want more hands-on training.
Other presentations and workshops at this year’s conference include ones on obstetrics, Aboriginal healthcare, procedural sedation, airway management, suturing and ultrasound.
For more information or for registration information, check out the RECC 2016 information brochure.
A GP for Me Work
Gabriola’s Most Vulnerable Benefit from Social Worker Position
If variety is the spice of life, then Angela Pounds’ life is spicier than most.
As part of a pilot funded by a GP for Me grant, she’s been kept busy this past year as the community social worker on Gabriola Island. Her caseload includes clients from 19 to 80 years old and everything in between. She liaises with schools, the RCMP, health care providers, advocacy groups and the food bank. And she helps with a range of client issues, from housing to finances to children and family issues.
“As part of our team, she’s helping enhance general wellness,” says physician lead Dr. Tracey Thorne, “by filling in the gaps in care for vulnerable members of our community.”
Working out of the Gabriola Medical Clinic and the social services agency, People for a Healthy Community, Pounds hit the ground running when she first started a year ago and the referrals haven’t stopped since. “Sometimes, the reasons people end up at the doctor aren’t medical at all, but rooted in financial or social concerns,” says Pounds. “The doctors always want to help, but they are extremely busy and, as a registered social worker, there’s a lot that I can take off their hands. This position lets the doctors concentrate on the actual doctoring.”

Pounds cites a recent example in which she was referred to an elderly gentleman who was becoming increasingly isolated after his wife died. “I went to see him and it turns out he needs hearing aids, which he couldn’t afford. So I contacted the Lions Club, which has an affordable hearing aid program. Now he can hear again, which is a vital part of staying social.”
In another case, a clinic doctor referred her to an elderly patient who wasn’t taking his medication because he couldn’t afford it. Pounds worked with the Ministry of Social Development and Social Innovation to get his medical benefits reinstated so he could afford the drugs he’d been prescribed.
During the pilot, Pounds saw, on average, between10 and 20 such clients each week. Its success, she says, had a lot to do with teamwork.
While the pilot itself wraps up in May 2016, Pounds will continue in her position as community social worker, thanks to the support of Island Health. That can only be welcome news for Gabriola residents—and the people who take care of them.
Adult Day Program Fills Gap in Care:
Ability-based Approach Gives a Boost to Port Hardy Seniors
It’s not often that we get to witness a transformation. But that’s exactly what happened during a recent Adult Day Program pilot in Port Hardy targeting vulnerable seniors and their caretakers.
Close to 100 people, many in their 80s and 90s with limited mobility and living with home health care, participated in the 10-week program—with remarkable results.
Seniors, Caretakers Benefit
They would arrive at the Hardy Bay Seniors’ Centre to coffee, tea and lively talk around a big table. Next up, a chance to move, to stretch or strengthen little-used muscles during a variety of exercise classes. Finally, a shared meal and some fun brain games.
For many it would be the only time they left the house in a week, the first time in a long time they would feel socially, physically, cognitively and emotionally engaged. For the caretakers, who knew their loved ones were in good hands, it was an opportunity to take a much-needed break.
The program was designed to fill a very real gap in care, says physician lead Dr. Dave Whittaker. “We see the breakdown in care when these folks end up in the ER in distress. As physicians, we try to help, but there’s very little we can do.”
The pilot wasn’t just about providing a nutritious meal, adds Dr. Whittaker. “I sat in on a session one day and it was amazing to see how important the interaction, the social part of this program, was. It had an immediate impact.”
Improving Quality of Life
That’s exactly what Angelina Passarelli, a Certified Therapeutic Recreation Specialist, hoped for when she developed and delivered the pilot. “Older adults face significant barriers in smaller communities, one of them being transportation, and it’s easy to become isolated. Our main goal was to enhance quality of life for these folks by reducing the isolation, by bringing them together in one place, where they could interact with others and exercise the mind, body and soul. Most importantly, they could reconnect with their former selves, embracing their abilities despite their disabilities, thereby creating new identities.”

Positive Feedback
Clearly, the program met its goals. In a survey, one caretaker writes of her elderly neighbor, who participated in the pilot: “For the first time in over seven years, he feels like a valued person instead of a problem that needs to be dealt with…The program has brought life and light and joy into his life.”
A home health care worker had this to say: “I saw some clients that seemed withdrawn in their homes come out of their shells and become very social.”
One younger participant with MS writes: “I so needed this program. Without it I would probably just sit at home and watch TV. Another writes: “The program provided assistance, encouragement and positive reinforcement on so many levels.”
Next steps are to try the program in other small communities, says Dr. Whittaker. “With such fantastic feedback, we’ve shown enough value to try and make it a sustainable model.”
Perspectives
2nd Annual Rural Locum Forum Reflects Supportive Locum Community
For young locum, Dr. Kimchi Nguyen, R&R Division’s 2nd annual Rural Locum Forum in Nanaimo in February was an opportunity to speak about her present—and to see into her future.
She was part of the opening panel discussion titled, “Striving and Surviving as a Rural Locum Physician,” and she spoke about what it’s like to be an early-career locum in rural BC. She joined two other opening panel presenters; Dr. Sandra Lee, who talked about her experiences as a middle-career locum, and Dr. Doug McTaggert, who provided a veteran’s perspective of rural family medicine.
Dr. Nguyen, who attended the very first Forum during her last year of residency, says this year she was impressed with the range in age and career scope of Forum participants.
“I met locums from smaller communities in every corner of the province,” she says, “and I could see all the opportunities out there. My eyes were also opened to the potential mentorship and support there is in the locum community. As a young physician just out of residency, the clinical courage that typically comes with years of work experience is difficult to come by. To have a network of experienced physicians like this who you can look to for support is just so valuable.”
Talking with other locums of all ages and times in their career paths confirmed for Nguyen that she’s headed in the right direction. “I realized I like serving smaller communities by providing relief for rural doctors who really need it. I like the mix of family practice, emergency, and hospital medicine. And I like the opportunity for travel that being a locum provides. While there are certainly challenges to being a rural locum, we’re bound together by what we do and this Forum was the perfect environment for all of us to connect.”



