Welcome to the Rural and Remote Division of Family Practice
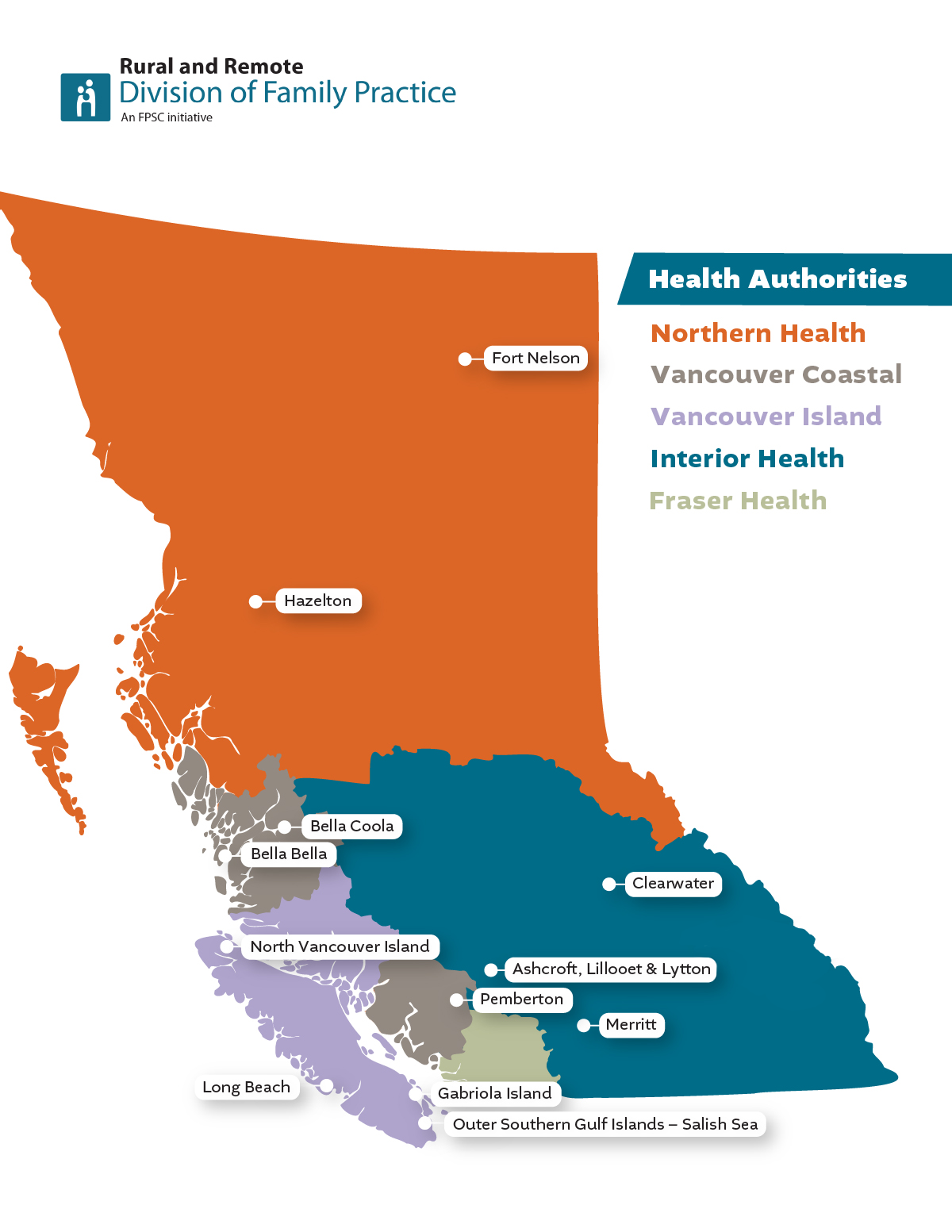
Our mission is to empower rural and remote primary care providers by connecting them with resources, improving their well-being, reducing isolation, and fostering innovation to strengthen equitable, culturally-safe healthcare across BC's rural and remote communities. Established in 2012, the Rural and Remote Division of Family Practice supports more than 150 physicians and nurse practitioners in 12 chapters across the province. Our Division works with four geographic Health Authorities and the First Nations Health Authority in more than 100 communities across the province, including more than 50 Indigenous communities. Our members serve approximately 140,000 patients over approximately 100,000 kilometers squared.
Together, we advance member priorities locally, across communities, and provincially. Have an interest in practicing in one of our communities? We'd love to meet you!